Bone tissue is made up of 70% inorganic components (45% mineral salts and 25% water) and 30% organic matrix. The 90% of this organic matrix is type I collagen to which the calcium salts are attached.
The special bond between collagen and calcium salts provides the bone a characteristic toughness and mechanical resistance.
During aging, the loss and deterioration of bone collagen causes the release of calcium salts (decalcification). Consequently, bone mass is reduced, and the bone becomes more fragile, increasing the risk of fracture.
When this process causes a marked and pathological loss of bone mass, it is called osteoporosis (OP), a silent disease until a fracture occurs. OP affects more women after menopause because the decrease in the level of estrogens slows down the synthesis of collagen1.

At this point, supplementing the diet with only calcium and vitamin D is not enough help because the calcium salts cannot reattach to the bone if its organic matrix does not have enough collagen fibers to adhere to.
That is why we need a supplement capable of nourishing both the mineral (calcium salts) and the organic (collagen matrix) components of bone tissue and stimulating its regeneration.
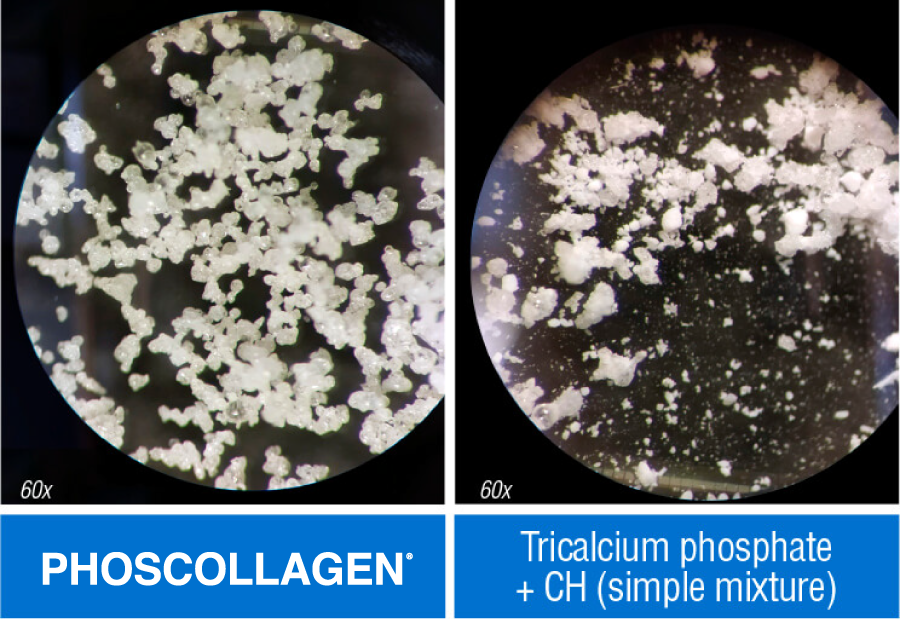
It is known that collagen peptides have a good mineral binding capacity that allows the formation of peptide-mineral complexes. This is the case of PHOSCOLLAGEN®, a peptide-mineral complex formed by COLPROPUR D® hydrolyzed collagen and hydroxyapatite (HAP, the bone-specific calcium phosphate salt), both of bovine origin, in which the micronized HAP is stabilized in a matrix of collagen peptides, forming a homogeneous ingredient that is not a simple mixture, but an uniform compound.
PHOSCOLLAGEN® brings together the nutritional and functional properties that a supplement needs to take care of bone health in an optimal and sustainable way:
In an in vitro study2 carried out with human osteoblast cultures treated with PHOSCOLLAGEN®, after simulating its gastrointestinal digestion and absorption, a significant increase in the proliferation of preosteoblasts (Fig. 1) and in the production of gene expression of bone biomarkers associated with the osteogenic activity of mature osteoblasts (Fig. 2) is observed at 24h in comparison with the control (sample resulting from digestive and absorption processes in the absence of PHOSCOLLAGEN®). These results show that PHOSCOLLAGEN® is a functional food ingredient useful for promoting bone formation.


Consistent with the results of PHOSCOLLAGEN® study, there are other studies that support the benefits of hydrolyzed collagen on bone health3-8 and show how its intake significantly improves the results of calcitonin administration9 and calcium and vitamin D supplementation10-15.
